There is always a risk whenever you undergo any cosmetic treatment, but with something as noninvasive and common as injectables, it’s hard to consider the possibility that something could go wrong. For former Shahs of Sunset star Lilly Ghalichi, something did go wrong, and she took to her Instagram account to share it with her followers.
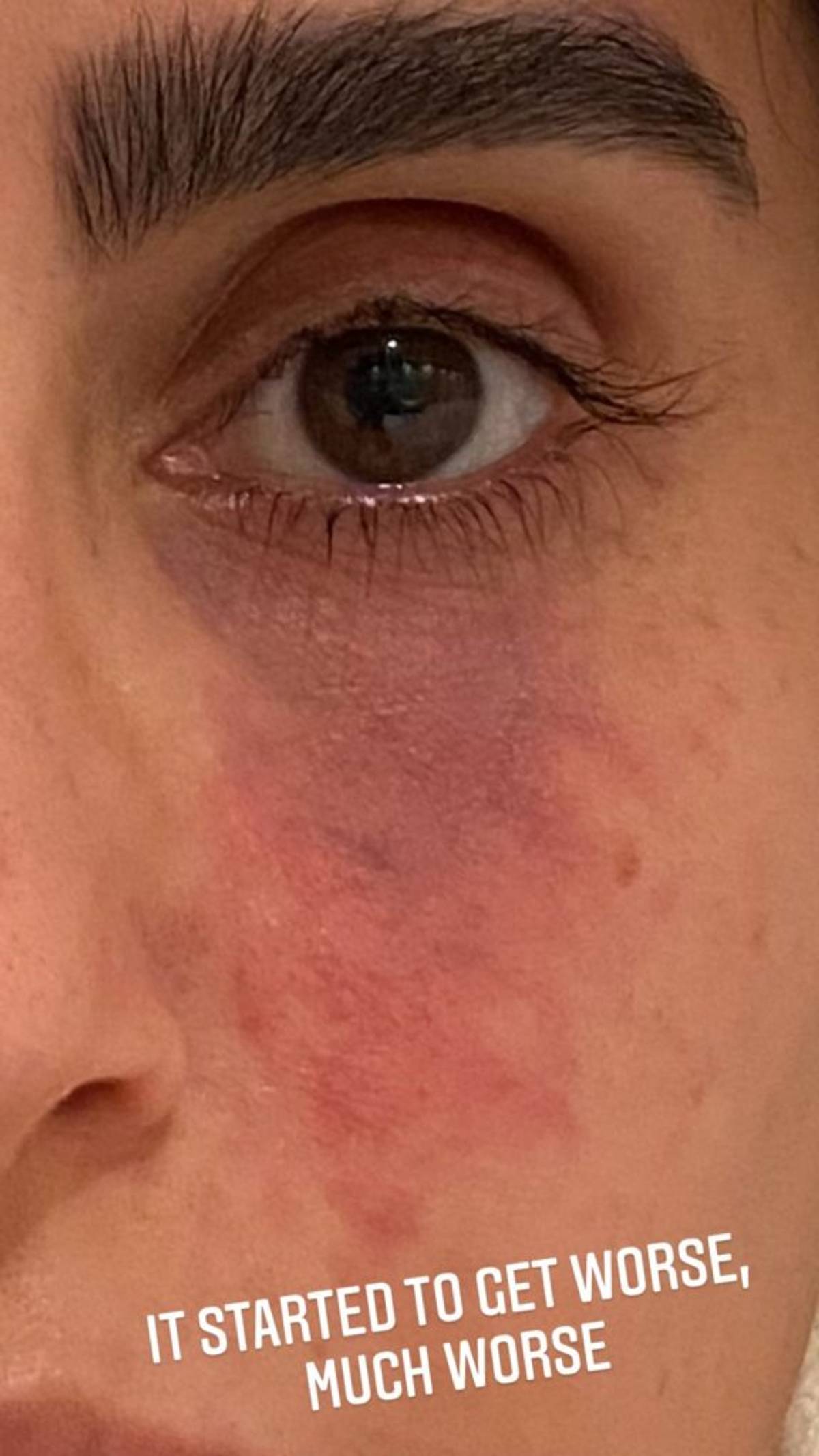
After receiving a bit of under-eye filler, Ghalichi started to notice that her skin appeared to be red and turning darker, as if it were bruised. Before she knew it, her skin began to get worse. What happened during her treatment is called Vacular Occlusion, which is caused by an accidental injection of filler into an artery.
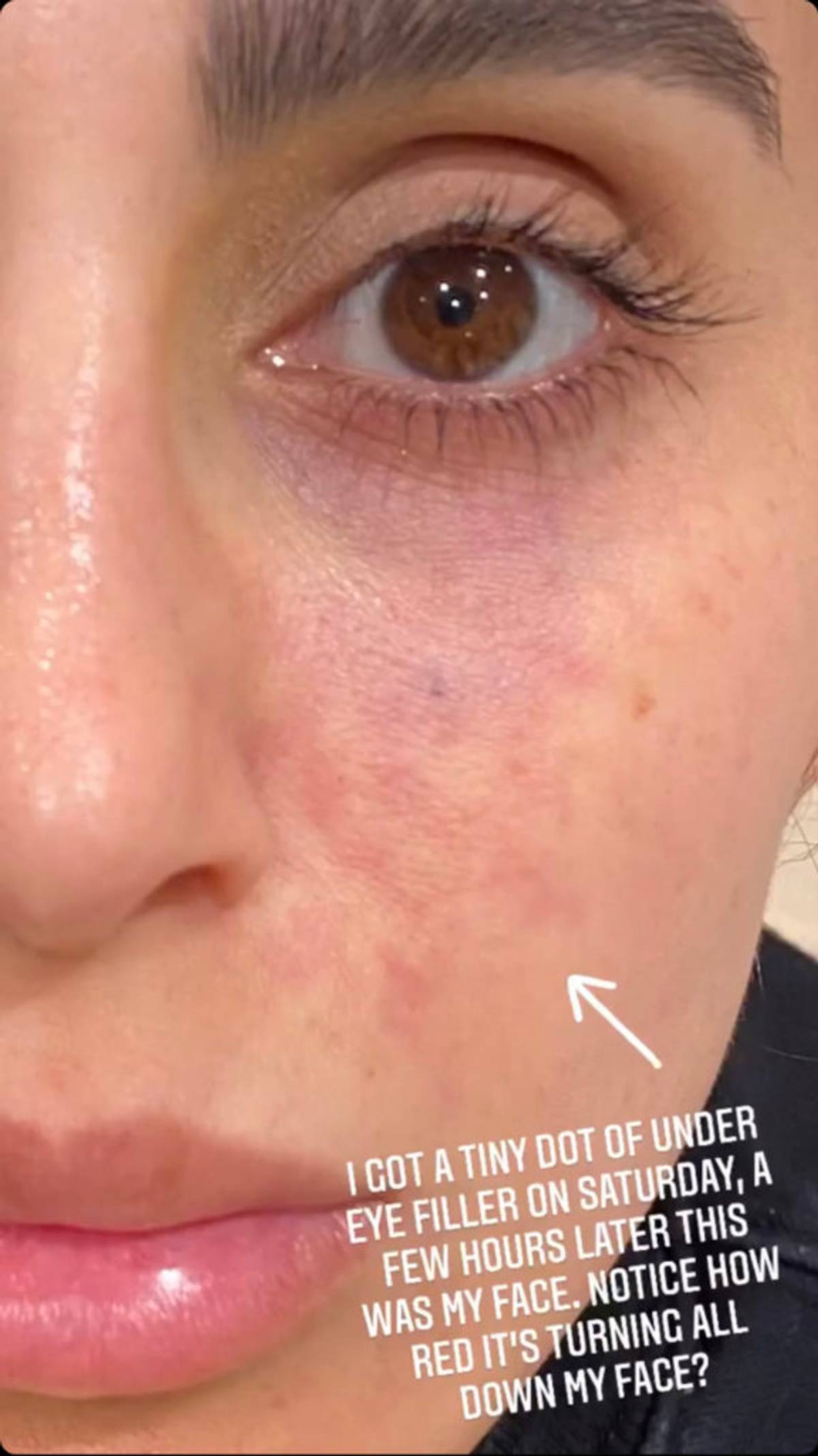
“I cannot speak to this specific case or patient as I was not involved in her care, but in general vascular occlusion is when filler is accidentally injected inside a blood vessel so that the tissue it supplies no longer receives oxygen or nutrients,” explains Campbell, CA dermatologist Amelia K. Hausauer, MD. “If this occurs without correction it can cause skin necrosis, meaning the skin can die, leaving a wound.”
“If the filler has been injected into a blood vessel or even if it's compressing, or pushing down on a blood vessel, it's not able to feed the skin with blood and then ultimately the skin starts to look muddled and bruised,” adds Fort Lauderdale, FL dermatologist Maryann Mikhail, MD. “Skin necrosis begins, and the skin turns black or blisters and starts sloughing off.”
Techniques Expert Injectors Use to Avoid It
The single most important thing in trying to minimize the risk of vascular occlusion is to find an expert injector who is very familiar with facial anatomy. “I did an extra year of advanced cosmetic training after medical school and dermatology residency,” says Dr. Hausauer. “One of the first things I had to do as a fellow was draw all the major blood vessels of the face on a patient from memory. Knowing the anatomy—location, depth, variation of blood vessels—allows for the safest techniques.”
Dr. Mikhail says techniques used while injecting is also helpful in avoiding an occlusion. “In addition to being familiar with facial anatomy, pulling back on the syringe every time you inject would be the second thing we do. Number three is using a cannula—specifically a larger gauge cannula. A cannula looks like a needle, but it has a blunt tip which is going to be a lot harder to penetrate a vessel, especially with a larger bore cannula.” To a certain point, Dr. Mikhail says it's not fully avoidable because the filler could be compressing a blood vessel, which can also cause this result.
Danger Zones
We have blood vessels all over our face, but the areas that are the most at risk are the nose, the glabella lines, the forehead, and nasolabial folds. “These are not common, but the face should be treated with great respect and attention to detail,” notes Dr. Hausauer.
“It can really happen anywhere,” says Dr. Mikhail. “Common places are the nasolabial folds, and close to the nose there's the angular artery. It happens anywhere all around and along the back of the nose where there are many tiny little blood vessels, the lips and it can even happen in the glabellar complex around the eyes.”
Other Risks
Another rare or commonly reported adverse event caused by vascular occlusion is blindness. “Occasionally, there are also reports of filler moving backward in the bloodstream of vessels important for the eye and thus, causing vision changes or loss,” Dr. Hausaur says. “This is the most severe risk of filler and extremely rare.”

Immediate Treatment
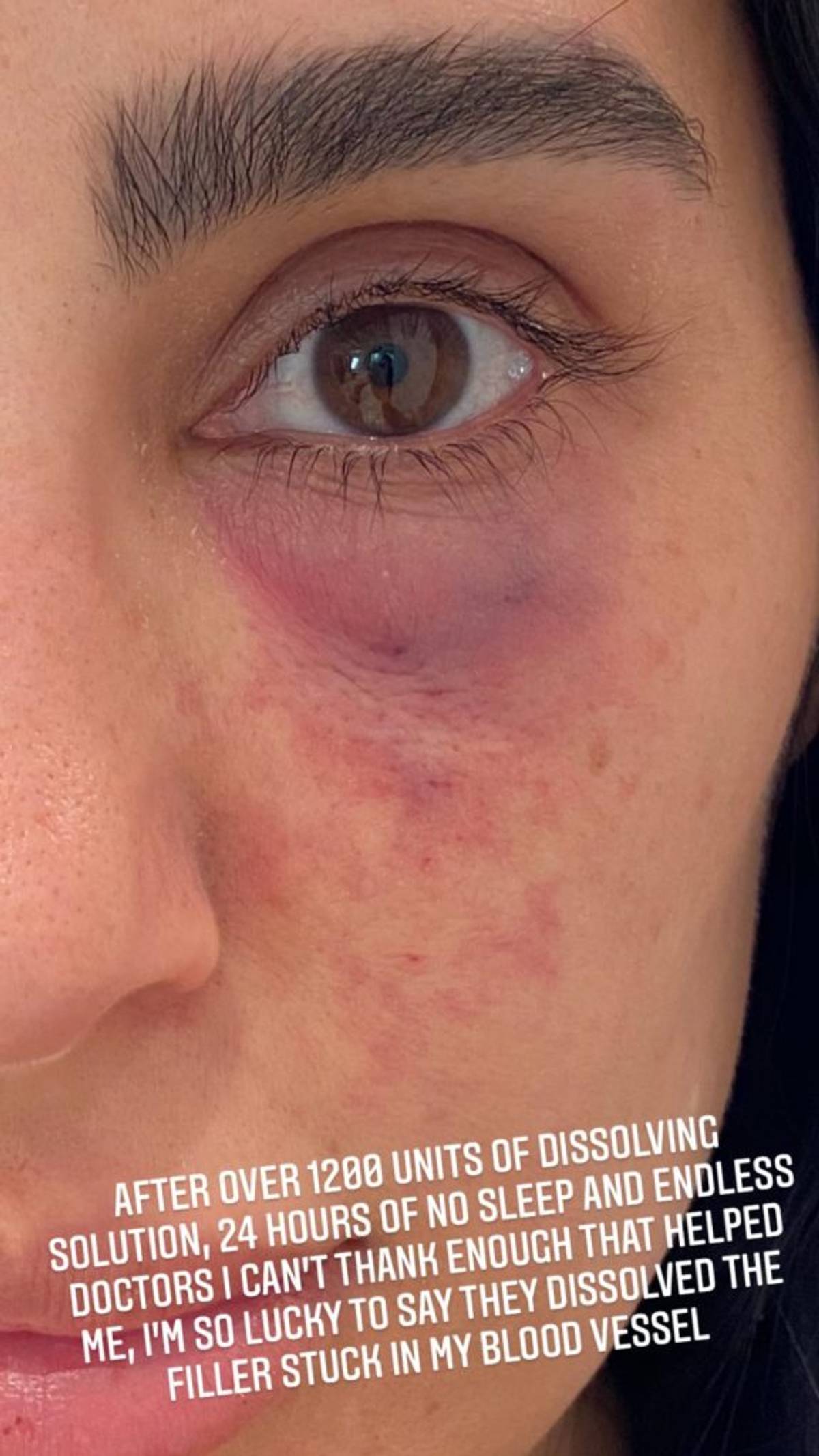
As Ghalichi shared on her IG stories, to save her skin, she and her doctor had to act fast. To treat this concern, dissolving the filler quickly is the key to ensuring the skin does not die. “As an injector, you see blanching so immediately,” notes Dr. Mikhail. “If you see like the blood rush out of the skin in the area that's your first clue that it happened. You have to stop injecting immediately, get the hyaluronidase which dissolves hyaluronic acid filler, and inject it until you see the profusion come back. If you catch it in time and the skin hasn’t died, you see the blood come down to the skin and it starts to heal.”
Hyaluronidase and a quick response saved Ghalichi’s skin. “Thank you to the filler response team at UCLA who helped save my skin, and asked I share my story to help others become aware of the very real risk of fillers,” wrote the reality star as she shared her story which thankfully now has a happier ending.


















